Medicine and Treatment for
Diabetes in Murfreesboro, TN
Medicine and Treatment for Diabetes in Murfreesboro, TN
Diabetes
You should never take diabetes lightly. This disease took over 102,188 lives in 2020, making it the seventh leading cause of death in the nation. It’s the No. 1 cause of kidney failure, adult blindness, and amputations. At Highland Family Medicine, Dr. Helton, Dr. Housden, and Dr. Hardin work together to provide you with the best treatment for diabetes type 1 or 2. If you have these early signs, such as constant hunger, fatigue, frequent urination, blurred vision, and sudden weight loss, schedule an appointment with us as soon as possible.
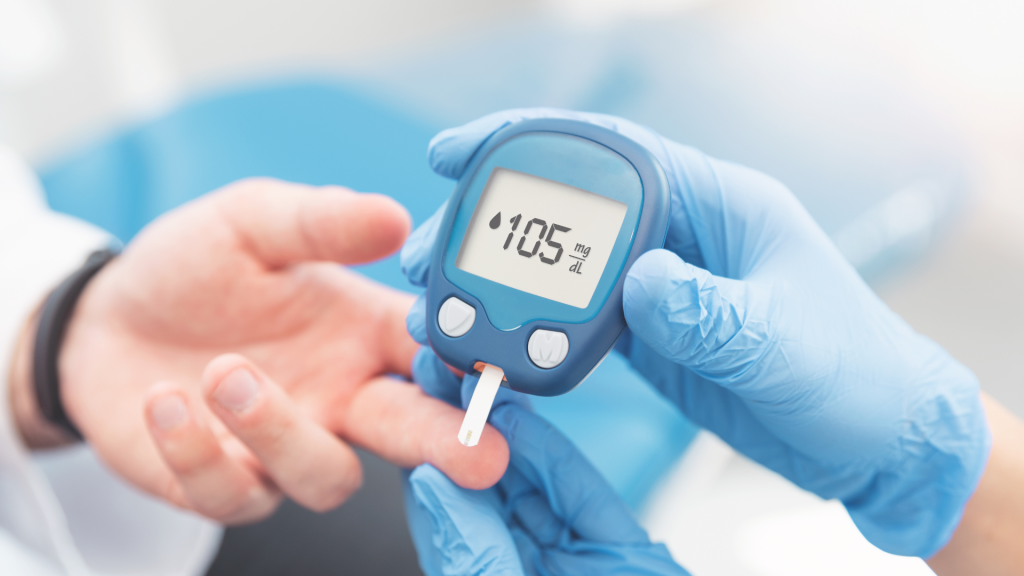
Diabetes is one of the world’s deadliest chronic diseases. It occurs when the pancreas can no longer make insulin, or the body cannot make good use of the insulin it produces.
Insulin is a hormone made by the pancreas, and it acts like a key to let glucose from the food we eat pass from the bloodstream into the cells in the body to produce energy. The carbohydrates we take are broken down into glucose in the blood. Insulin helps glucose get into the cells.
Not being able to produce insulin or use it effectively leads to raised glucose levels in the blood (known as hyperglycemia). Over the long-term high glucose levels are associated with damage to the body and failure of various organs and tissues.
Type 1 and Type 2 Diabetes
When your primary care physician tells you that you have type 1 diabetes, it means that it’s a genetic condition. The early signs and symptoms of type 1 diabetes show up early in life, as young as four to seven years old. However, it may still occur later in life. Type 2 diabetes, on the other hand, is a condition due to lifestyle-related and progresses over time.
Type 1:
Your body attacks your pancreas, hindering it from creating insulin (autoimmune disease)
Type 2:
Your body becomes no longer capable of making enough insulin, or the insulin you do make doesn’t work properly
Both types share similar symptoms. However, treatment for each type differs significantly. Type 1 is arguably worse because you are born with it, and there’s nothing much you can do about it but comprehensive food management and medication. With type 2 diabetes, you can change your lifestyle and be consistent, improving the odds of putting your diabetes into remission.
Both types technically do not have a cure. However, type 2 can go into remission, whereas type 1 cannot.
Symptoms of Diabetes vary depending on the level of blood sugar elevation. Some people, especially those with prediabetes or type 2 diabetes, may not experience symptoms initially.
Type 1 diabetes, symptoms tend to come on quickly and be more severe.
Some of the signs and symptoms of type 1 and type 2 diabetes are:
- Increased thirst
- Frequent urination
- Extreme hunger
- Unexplained weight loss
- Presence of ketones in the urine (ketones are a byproduct of the breakdown of muscle and fat that happens when there’s not enough available insulin)
- Fatigue
- Irritability
- Blurred vision
- Slow-healing sores
- Frequent infections, such as gums or skin infections and vaginal infections
Diabetes, if not diagnosed and treated early, will impose long-term complications which develop gradually. The lesser controlled your blood sugar level is and the longer you have diabetes — the higher the risk of complications. Eventually, diabetes complications may be disabling or even life-threatening. Possible complications include:
Cardiovascular Disease
Cardiovascular disease is the most common complication of diabetes, which is the risk of various cardiovascular problems, including coronary artery disease with chest pain (angina), heart attack, stroke, and narrowing of arteries (atherosclerosis). If you have diabetes, you’re more likely to have heart disease or stroke.
Nerve Damage (Neuropathy).
Excess sugar can injure the walls of the tiny blood vessels (capillaries) that nourish your nerves, especially in your legs. Neuropathy can cause tingling, numbness, burning, or pain that usually begins at the tips of the toes or fingers and gradually spreads upward.
Left untreated, you could lose all sense of feeling in the affected limbs. Damage to the nerves related to digestion can cause problems with nausea, vomiting, diarrhea, or constipation. For men, it may lead to erectile dysfunction.
Kidney Damage (Nephropathy)
The kidneys contain millions of tiny blood vessel clusters (glomeruli) that filter waste from your blood. Diabetes can damage this delicate filtering system. Severe damage can lead to kidney failure or irreversible end-stage kidney disease, which may require dialysis or a kidney transplant.
Eye Damage (Retinopathy)
Diabetes can damage the retina’s blood vessels (diabetic retinopathy), potentially leading to blindness. Diabetes also increases the risk of other serious vision conditions, such as cataracts and glaucoma.
Foot Damage
Nerve damage in the feet or poor blood flow to the feet increases the risk of various foot complications. If foot damage is left untreated, cuts and blisters can develop serious infections, which often heal poorly. These infections may ultimately require toe, foot, or leg amputation.
Skin Conditions
Diabetes may leave you more susceptible to skin problems, including bacterial and fungal infections.
Hearing Impairment
Hearing problems are more common in people with diabetes.
Alzheimer’s Disease
Type 2 diabetes may increase the risk of dementia, such as Alzheimer’s disease. The poorer your blood sugar control, the greater the risk. Although there are theories about how these disorders might be connected, none has yet been proven.
Depression
Depression symptoms are common in people with type 1 and type 2 diabetes. Depression can affect diabetes management.
Most women who have gestational diabetes deliver healthy babies. However, untreated or uncontrolled blood sugar levels can cause problems for you and your baby.
Complications in your baby can occur as a result of gestational diabetes, including:
- Excess growth. Extra glucose can cross the placenta, which triggers your baby’s pancreas to make extra insulin. This can cause your baby to grow too large (macrosomia).
- Larger babies are more likely to require a C-section birth.
- Low blood sugar. Sometimes babies of mothers with gestational diabetes develop low blood sugar (hypoglycemia) shortly after birth because their own insulin production is high. Prompt feedings and sometimes an intravenous glucose solution can return the baby’s blood sugar level to normal.
- Type 2 diabetes later in life. Babies of mothers who have gestational diabetes have a higher risk of developing obesity and type 2 diabetes later in life.
- Death. Untreated gestational diabetes can result in a baby’s death either before or shortly after birth.
Complications in the mother also can occur as a result of gestational diabetes, including:
Preeclampsia
This condition is characterized by high blood pressure, excess protein in the urine, and swelling in the legs and feet. Preeclampsia can lead to severe or life-threatening complications for both mother and baby.
Subsequent Gestational Diabetes
Once you’ve had gestational diabetes in one pregnancy, you’re more likely to have it again with the next pregnancy. You’re also more likely to develop diabetes — typically type 2 diabetes — as you get older.
Diabetes is a chronic disease that you cannot treat at home. Our doctors will help you make a diabetes treatment plan that is right for you — and that you can understand. You may also need other healthcare professionals on your diabetes treatment team, including a foot doctor, nutritionist, eye doctor, and diabetes specialist (called an endocrinologist).
Treatment for diabetes requires serious tracking of your blood sugar levels (and keeping them at a goal set by your doctor) with a combination of treatment options like medications, exercise, and diet. By paying close attention to your diet and lifestyle, you can minimize or avoid the “seesaw effect” of rapidly changing blood sugar levels, which can require quick changes in medication dosages, especially insulin.
Type 1 Diabetes Treatment:
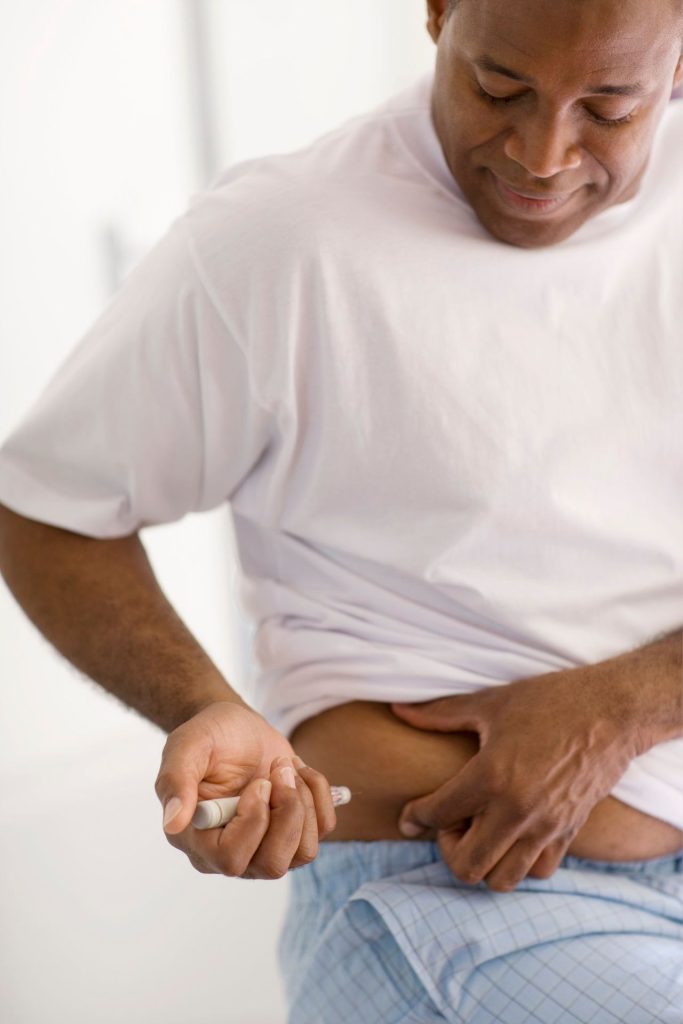
Insulin injections are the main treatment for type 1 diabetes, and they come in several different forms, with each working slightly differently. Some last up to a whole day (long-acting), some last up to eight hours (short-acting), and some work quickly but don’t last very long (rapid-acting). You’ll most likely need a combination of different insulin preparations.
There are alternatives to insulin injections, but they’re only suitable for a small number of patients. They are:
- Insulin pump therapy – where a small device constantly pumps insulin (at a rate you control) into your bloodstream through a needle that’s inserted under the skin
- Islet cell transplantation – where healthy insulin-producing cells from the pancreas of a deceased donor are implanted into the pancreas of someone with type 1 diabetes
Complete pancreas transplant
Type 2 Diabetes Treatment
You have many options to manage type 2 diabetes. Diet, exercise, and medication work together to bring your blood sugar under control.
Your doctor will help you determine if you need to take medicine, which kind is right for you, and how often you should take it.
Over your lifetime, you’ll probably handle your disease in different ways. Sometimes medications stop working, and you’ll have to switch. You’ll need to adjust to changes in your body as you age. And researchers are looking for new diabetes medicines and ways to treat it.
- Healthy Eating
- Lifestyle Change
- Regular exercise
- Diabetes medication or insulin therapy
- Blood sugar monitoring
Request an Appointment
The Highland Family Medicine Diabetes Care
According to the 2018 America’s Health Ranking’s Annual Report, Tennessee has over 650,000 diabetic adults (13.1% of the population), and around 250,000 are undiagnosed. We know how difficult it is to manage diabetes, and that’s why Dr. Helton and fellow family doctors work hard to help the community by offering more than just medication.
Highland Family Medicine provides guidelines and advice to help you manage your diabetes effectively through proper diet and exercise. We also educate you on what foods to avoid and what will keep you healthy. It is a challenge to restrain, but together, we can find a system to help you manage your condition and live a healthy, normal life with the hopes that your diabetes will go into remission.


Highland Family Medicine and its doctors, Dr. Helton, Dr. Housden, and Dr. Hardin, have been serving and treating the community of Murfreesboro, TN, and surrounding areas for over two decades.
Collectively, they have treated more than 20,000 patients. Highland Family Medicine specializes in comprehensive health care for people of all ages, treating most ailments and non-emergencies.
Please don’t hesitate to call the Highland Family Medicine doctor’s office. Dr. Helton, Dr. Housden, and Dr. Hardin are professionals and ready to serve.
